In Vitro Fertilization (IVF) is the most effective medical solution for couples and women who face infertility, offering a real chance to achieve pregnancy with the help of modern technology and specialists in assisted human reproduction.
This complex procedure includes: stimulation of the ovaries, egg retrieval, fertilisation in the laboratory and transfer of the embryo into the uterus, in a controlled and safe environment.
It is estimated that more than 95% of infertility cases can be treated, and IVF represents one of the most advanced and effective methods available today, with clinically proven results and increased chances of success from the very first attempt.
Through personalised medical care and an integrated approach, Genesis Athens offers patients access to the most modern assisted reproduction treatments, tailored to each individual case.
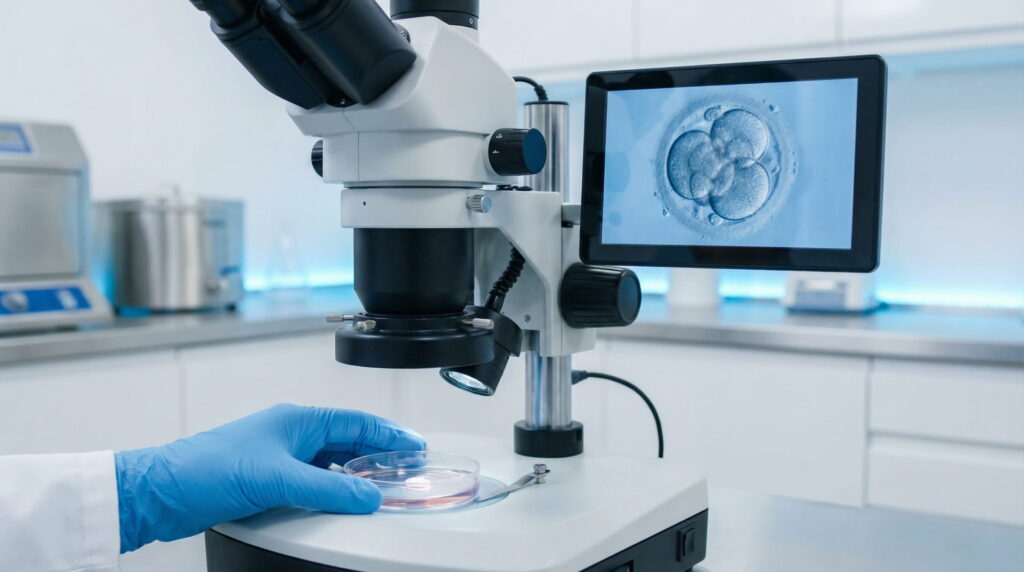
What Is In Vitro Fertilization (IVF)
In vitro fertilization (IVF) is a method of assisted human reproduction in which the female reproductive cell is brought into contact with the male reproductive cells in the laboratory. Fertilisation takes place in vitro, but in a way that is identical to what happens in the fallopian tubes (in vivo).
The IVF procedure is different from intrauterine insemination (IUI), where active sperm cells are injected into the uterus through a catheter. This assisted reproduction treatment brings the sperm as close as possible to the egg, thereby improving the chances of fertilisation.
When Is the IVF Procedure Recommended
In vitro fertilization (IVF) is recommended in the following diagnoses:
- Tubal infertility: obstruction of the fallopian tubes (blocked tubes), absence of the fallopian tubes
- Endometriosis
- Decreased ovarian reserve (few eggs remaining in the ovaries)
- Male infertility (poor semen parameters)
- Failure of previous intrauterine insemination cycles
- Unexplained infertility
Stages of the IVF Procedure
The IVF procedure is carried out in several stages: ovarian stimulation, egg collection, fertilisation of the eggs with sperm from the husband or chosen donor, followed by transfer of the embryo into the uterus of the future mother.
The major advantage of IVF is the possibility of performing genetic testing on the resulting embryo, allowing the detection of abnormalities before it is implanted in the uterus.
The younger the woman, the higher the success rate of an IVF cycle. Advanced female age dramatically decreases the chance of success of in vitro fertilization, because of ovarian depletion, reduced egg quality and a weaker response to stimulation.
At Genesis Athens, the success rate from the very first IVF procedure is over 57%.
Stage 1: Initial Evaluation and Fertility Tests

A rigorous diagnosis of infertility and a personalised treatment plan are basic conditions for the success of any in vitro fertilization treatment.
The first test is the semen analysis (spermogram).
The woman’s tests include hormonal tests, transvaginal ultrasound and, where appropriate, genetic tests.
Stage 2: Controlled Ovarian Stimulation
After the diagnostic workup, the first stage of the IVF procedure is ovarian stimulation. The ovaries are stimulated with specific medication so that they mature all the eggs that can be brought to maturity in one month. Normally, the body can mature only one egg per month. The other eggs that start to mature during that month are lost. Through ovarian stimulation, these eggs are not lost.
The egg is protected by a follicle, a small fluid-filled sac. The follicle can be seen on ultrasound. Monitoring the number and growth of follicles during treatment is carried out by transvaginal ultrasound and blood hormone tests.
These tests make it possible to determine the optimal time for egg retrieval.
The combination of medications used to induce and mature follicles, the so-called synthetic gonadotropins, as well as their dosage and the type of therapy, are adapted and individualised according to the patient’s age, her ovarian response and the needs of each couple.
One possible risk during hormonal treatment is a lack of response to the medication.
Lack of response to treatment occurs especially in patients of advanced age and with decreased ovarian reserve, and is quantified by the development of an insufficient number of ovarian follicles or by their insufficient maturation.
If the problems cannot be solved by increasing the doses of medication, egg donation is recommended.
The couple needs to understand that starting ovarian stimulation treatment does not guarantee egg retrieval. In some patients, the medication may not produce the expected reactions of follicular growth and maturation. However, these aspects will be explained in detail during the medical consultation.
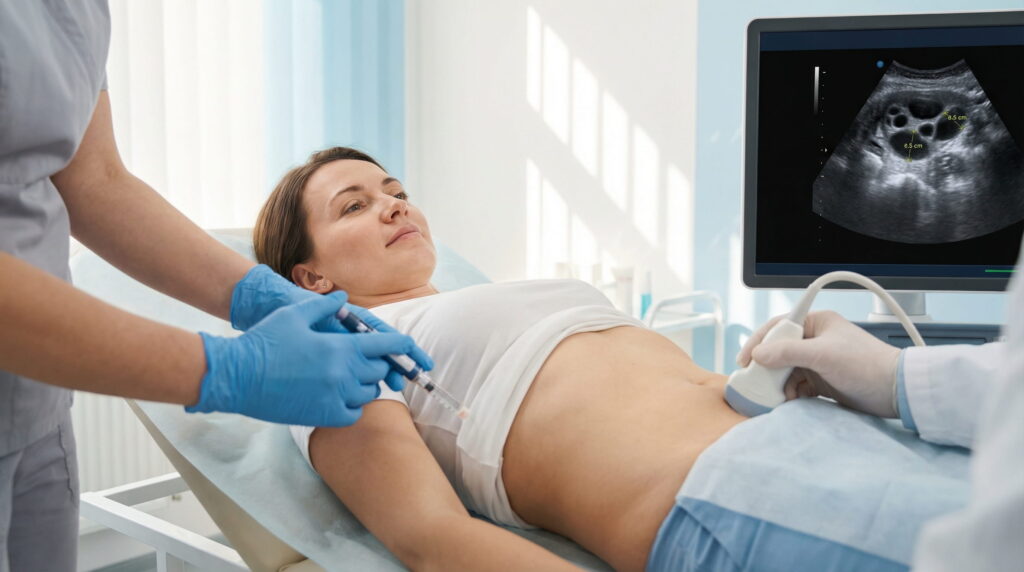
Stage 3: Egg Collection (Ovarian Puncture)
Egg collection is performed after completion of follicular maturation monitoring, by transvaginal follicular puncture.
Egg retrieval is carried out under ultrasound guidance. It is a short, painless procedure that can also be observed by the husband.
On request, mild sedation or general anaesthesia can be used. If in your case anaesthesia is contraindicated, egg retrieval can also be performed without anaesthesia.
On the day of egg retrieval, it is recommended that you come to the clinic together with your partner at least half an hour before the scheduled time. On the evening before, you should not eat. Before the procedure, you should avoid drinking water, coffee, or consuming chewing gum or sweets, in order to prevent nausea and vomiting.
After egg retrieval, you can eat normally. It is preferable, however, to start with fluids, such as water or orange juice, and to choose light food.
After egg retrieval, you may have brown vaginal discharge.
You may also feel some discomfort and mild pain in the lower abdomen, but you should not be worried, because these reactions are normal.
It is also possible for your temperature to be around 37.3 °C. If you feel that you have a fever, you should measure it and inform your doctor.
Stage 4: Laboratory Fertilisation
The eggs, collected by the embryologists from the follicular fluid, are placed in a special culture medium in incubators.
Immediately after egg retrieval, the husband must provide a semen sample. If the man has difficulties in providing the sample at that time, semen previously collected on earlier days can be used.
The semen must be renewed (through masturbation or sexual intercourse). It is provided by the husband at the clinic or can be brought from home, after being collected in a sterile container.
There are two methods of in vitro fertilization that can be performed in the laboratory:
In Vitro Fertilization (Conventional IVF)
The first method is relatively simple. The egg is brought into contact with a large number of sperm cells, and one of them will penetrate the protective zona pellucida of the egg and fertilise it.
A few hours after egg retrieval, and after the semen has been processed to remove prostatic fluid and select sperm cells with good motility, these sperm cells are placed together with the eggs in the culture medium (conventional IVF).
ICSI
The second method, ICSI (intracytoplasmic sperm injection), is used in cases of male infertility (oligospermia).
If there are problems related to the number or motility of sperm cells, fertilisation can be achieved using special techniques.
At present, the technique widely used is intracytoplasmic sperm injection into the egg, known as ICSI, made possible by scientific advances and technological progress.
This technique makes it possible to use the husband’s sperm even in severe cases of male infertility caused by an insufficient number of sperm cells, reduced motility of the semen or complete absence of sperm cells in the ejaculate (azoospermia).
In the past, the only solution for couples in which the man had such infertility problems was the use of donor sperm.
ICSI can also solve cases in which there are enough sperm cells quantitatively, but which, for unknown reasons, cannot achieve fertilisation by the conventional in vitro fertilization method.
In men who suffer from total azoospermia (absence of sperm cells in the ejaculate), it is possible to retrieve sperm cells from the epididymis (PESA) or from the testicle (TESA) using a fine needle under local anaesthesia.
Intracytoplasmic sperm injection is, in fact, a microscopic surgical intervention on the egg. With the help of a very powerful microscope, a sperm cell is captured with a micropipette. It is then introduced into the egg by creating an opening in the outer protective membrane of the egg, more precisely in its transparent zone, the zona pellucida. This membrane protects the egg and the newly formed embryo during its first days of life.
Usually, 2–3 days after embryo transfer, the zona pellucida dissolves and the free embryo can implant in the endometrium (in the uterus).
When the outer membrane is thick or very hard, the embryo cannot easily free itself. In such cases, shortly before embryo transfer, an artificial opening of the zona pellucida is made with the help of a laser under the microscope (assisted hatching). This method is minimally invasive and is most often required in women over 40 years of age. Assisted hatching helps the embryo implant efficiently in the uterus and increases the chances of success of fertilization.
Checking Fertilisation
Sixteen to twenty hours after IVF procedures, fertilisation is checked. If fertilisation has been successful, two pronuclei (two round structures) can be seen inside the egg under the microscope.
The Embryology Department will inform you about the number of fertilised eggs and the day and time when embryo transfer will be possible. The embryos are kept in culture until they reach the morula or blastocyst stages, which significantly increases the chances of achieving pregnancy. Not all embryos reach these stages, only the healthiest ones, approximately 4 out of 10, which results in a natural selection of vigorous embryos.
Stage 5: Embryo Culture and Embryo Transfer
Day 3 Embryos
At this stage, the cells inside the embryos divide but do not increase in size, maintaining the size of an unfertilised egg. On day 3, the embryologist uses a high-power microscope to evaluate the morphology (structure) of the embryo. The main elements of interest are the number of cells in the embryo and their appearance.
An embryo that divides well should ideally have between 6 and 10 cells on day 3. Eight cells is optimal.
Day 3 embryos are graded from 1 to 4 (or 5), depending on the laboratory’s protocol, with 1 being the highest grade.
Day 5 Embryos
On day 5, the embryo has around 80 cells and is called a blastocyst. At this stage, the embryologist has more information about the embryos that have successfully passed day 3 (some embryos stop developing).
Blastocyst grading is complex and is performed based on several parameters, using grades from 1 to 6 and letters (A, B or C), where A represents the best quality.
What is important to remember is that the grades obtained by blastocysts and the categories in which they are classified can change.
High grades do not guarantee success.
Studies show that embryos with higher grades are associated with better pregnancy rates and more live births, while embryos with lower grades are associated with lower pregnancy rates and fewer live births, but not in every case.
The conclusion is that it is difficult to predict success or failure based solely on these grades, and that you should certainly not lose hope.
With regard to the number of embryos transferred, this will be decided after a prior discussion between the couple, the doctor and the embryology specialists, taking into account the couple’s history, the woman’s age, the number of attempts already made to achieve a pregnancy, and the risk of multiple pregnancy.
Because a multiple pregnancy is associated with important gynaecological and perinatal complications (such as miscarriage or prematurity), as well as significant emotional and economic costs for the couple, it is preferable to transfer as few embryos as possible, without reducing the probability of success of the method.
If there is a higher number of resulting embryos, they can be preserved by freezing (cryopreservation) so that the couple can use them in the future. The benefit of cryopreservation is threefold: medical, psychological and economic. It avoids the need for a new ovarian stimulation with medication, a new egg retrieval and another in vitro fertilization cycle.
Embryos can be cryopreserved even at the blastocyst stage. After thawing, the survival rate of embryos is approximately 80%. Research has shown that pregnancies obtained from frozen embryos do not differ from those achieved using fresh embryos obtained immediately after puncture and fertilisation.
Embryo Transfer
After fertilisation, the resulting embryo is transferred into the uterus and placed at its base. Embryo transfer is a completely painless procedure that does not require any form of anaesthesia and is carried out using a special device (catheter).
Embryo transfer can be performed on days 2–3 (morula stage) or on days 5–6 (blastocyst stage), depending on embryo quality and the doctor’s assessment.
What Is Allowed and What Is Not After Embryo Transfer
Immediately after embryo transfer, a period of rest is recommended.
Some patients may experience mild cramping and slight bleeding.
As a rule, recommendations for women who have just completed the stages of in vitro fertilization are to avoid intense physical effort for 2–3 days after embryo transfer. It has not been proven that strict, prolonged bed rest helps embryo implantation in the uterus (the embryo must attach to the uterine lining), but this rest is recommended especially for psychological reasons.
In the following two weeks, the main daily activities can be resumed, but in moderation.
This means that it is more prudent to avoid a very active lifestyle, such as gym workouts, running, swimming or other intense sports, as well as heavy physical work and lifting weights. Attention should also be paid to diet in order to avoid constipation or indigestion.
Warm showers are recommended instead of hot baths, and the use of internal sanitary tampons, alcohol consumption and smoking should be avoided, as well as taking any medication without consulting the specialist doctor.
There are no contraindications regarding the sleeping position of the future mother; what matters is that she has restful sleep, whether she sleeps on her side, on her back or on her stomach.
Psycho-emotional stress is another factor that every woman who is awaiting the result after embryo transfer should take into account. It is not easy, but it can be managed more easily if daily activities are resumed, whether that means returning to work or meeting family and friends.
Finally, increased attention is recommended to avoid infectious diseases, including common colds.
Stage 6: The Beta-hCG Test and Confirmation of Pregnancy
Twelve to fifteen days after embryo transfer, a blood test is performed to measure beta-hCG (human chorionic gonadotropin), which shows whether in vitro fertilization has been successful or not.
This is a period in which uncertainty, doubts, impatience to find out the result and anxiety are difficult to cope with for any woman who has just completed an IVF procedure.
The level of this hormone in the woman’s blood is checked by the pregnancy test. If the test is positive (above 10 units), another blood test will be carried out after 2–3 days to see whether the hormone level is increasing.
Along with these blood tests, estradiol and progesterone levels are measured, two hormones that are good indicators of the presence of pregnancy. If everything progresses normally, a vaginal ultrasound will be performed four weeks after embryo transfer.
The first ultrasound aims to confirm the pregnancy and to exclude:
- an ectopic pregnancy (which occurs when the fertilised egg implants outside the uterus)
- a molar pregnancy (an abnormality of the placenta caused by a problem that occurs at fertilisation)
- a blighted ovum (or anembryonic pregnancy – which occurs when the fertilised egg attaches to the uterus but the embryo does not develop), and to diagnose a multiple pregnancy
Gradually, the first positive signs of pregnancy appear: mild general malaise, nausea, weakness. The breasts gradually enlarge and the areolae around the nipples may become darker.
A pregnancy obtained through in vitro fertilization progresses in the same way as a naturally conceived pregnancy. As with spontaneous pregnancies, there is a risk of complications (gestational diabetes, placenta praevia or preeclampsia), especially if the patient is over 40 years old or has a multiple pregnancy.
At present, the success rate of in vitro fertilizations is increasing and brings hope back into the lives of couples diagnosed with infertility.
If the pregnancy test is negative, you will need to schedule an appointment with your doctor in order to understand the reasons for failure and to discuss future options.i va trebui să vă faceți o programare la medic, cu scopul de a afla motivele nereușitei și de a discuta despre perspectivele de viitor.
Chances of Success in In Vitro Fertilization

At Genesis Athens, the success rate from the very first IVF procedure is over 57%. Owing to technological advances, we have one of the highest success rates in Europe.
In Romania, the average success rate of an IVF procedure is 35–40%.
Factors That Influence IVF Success Rates
- The patient’s age
- Egg and sperm quality
- The quality of the laboratory
- Hormonal and nutritional support
- Preimplantation genetic testing (PGT-A)
“You deserve to be heard, seen, treated with respect, and supported throughout your life.”

Andreas Vythoulkas
Specialist in Obstetrics and Gynecology


Costs of the IVF Procedure
The costs of the procedure are divided into:
- Costs for the initial evaluation
- Costs of stimulation medication
- Costs of the IVF procedure itself
- Costs of embryo transfer
The financial support granted through the IVF Program 2025 amounts to 15,000 lei, in the form of two digital vouchers:
- 5,000 lei for the purchase of medication (stimulation medication costs)
- 10,000 lei for the in vitro fertilization procedure itself (IVF procedure costs)
The vouchers are valid for 12 months from the date of issue.
Risks and Medical Recommendations
Lack of Response to Medication
Lack of response to hormonal treatment occurs mainly in patients of advanced age and with decreased ovarian reserve, and is expressed through the development of an insufficient number of ovarian follicles or their insufficient maturation.
The couple must understand that starting ovarian stimulation treatment does not guarantee egg retrieval. In some patients, the medication may not produce the expected effects of follicular growth and maturation.
However, these aspects will be explained in detail during the medical consultation.
If the problems cannot be solved by increasing treatment doses, egg donation is recommended.
Ovarian Hyperstimulation Syndrome
This is a severe complication of ovarian stimulation, seen infrequently (3–5%) in young women and in those with micropolycystic ovaries. The ovaries increase in volume and more than 20–25 ovarian follicles develop.
Typical symptoms include abdominal pain, nausea, vomiting, breathing difficulties and impaired liver and kidney function. Severe cases require hospitalisation.
Multiple Pregnancy
Approximately 25–30% of pregnancies obtained through IVF are twin pregnancies, and about 5% are triplet pregnancies. Ectopic pregnancies or implantation of the embryo outside the uterus are very rare.
Each case is closely monitored medically so that all possible risks are reduced.
Embryo Failure
One frequent cause is a thin endometrium, which does not facilitate embryo implantation, as well as the presence of endometriotic cysts.
Another important cause of IVF failure is poor-quality embryos. Especially when the patient is over 35 years of age, preimplantation genetic tests are recommended.
Uterine problems such as endometrial polyps, fibroids and intrauterine adhesions (scar tissue or adhesions inside the uterine cavity) are another common cause of IVF failure.
An important chapter among the causes of IVF failure is thrombophilia, a clotting disorder that prevents embryo implantation or allows implantation only for a short period, followed by miscarriage. When correctly diagnosed, thrombophilia can be treated, increasing the chances of success of in vitro fertilization.
Asymptomatic viral or bacterial infections can reduce the chances of successful embryo implantation.
Autoimmune conditions, in which the body produces antibodies that “attack” the embryo and prevent its implantation, can also affect the outcome.
Vitamin D deficiency.
Progesterone levels that are too low.
At Genesis Athens, each case is closely monitored medically in order to minimise all possible risks.
Preparing for IVF: How You Can Increase the Chances of Success
The chances of success can be increased before the IVF procedure as follows:
- Optimising body weight and diet
- Quitting smoking and alcohol
- Managing stress and taking supplements recommended by the doctor
- A complete medical evaluation of both partners

Frequently Asked Questions
What is in vitro fertilization and who is it for?
In vitro fertilization (IVF) is the method of assisted human reproduction in which the female reproductive cell is brought into contact with the male reproductive cells in the laboratory. Fertilisation occurs in vitro, but in a way that is identical to what happens in the fallopian tubes (in vivo).
How many eggs are collected in one IVF cycle?
Depending on the woman’s age, in an optimal in vitro fertilization (IVF) cycle, 8–15 eggs are collected.
After how many days is embryo transfer done?
Embryo transfer is most often carried out on day 3 or day 5.
What medications are used for ovarian stimulation?
The medications are synthetic gonadotropins.
What are the real chances of success with IVF?
At Genesis Athens, the Center of Excellence in Infertility Treatment, the success rate from the very first IVF procedure is over 57%.
How long does a complete IVF cycle take?
The time needed for a complete in vitro fertilization (IVF) treatment ranges between 4 and 6 weeks.
Is the procedure painful?
No. However, during egg retrieval from the ovary, sedation can be used if desired.
What happens to the remaining embryos?
The embryos remaining after in vitro fertilization (IVF) can be frozen for future use, some of them being suitable for additional embryo transfers in the future. The benefit of cryopreservation is threefold – medical, psychological and economic. It avoids the need for a new stimulation cycle, a new egg retrieval and another IVF cycle.
Embryos can be cryopreserved even at the blastocyst stage. After thawing, the embryo survival rate is approximately 80%. Research has shown that pregnancies resulting from frozen embryos do not differ from those obtained with fresh embryos, created immediately after puncture and fertilisation.
However, at the family’s decision and according to legal regulations, the remaining embryos can also be discarded.

Why Choose Genesis Athens for In Vitro Fertilization
At Genesis Athens, the Center of Excellence in Infertility Treatment, the success rate from the very first IVF procedure is over 57%.
Genesis Athens is the largest infertility treatment center in Romania.
- We have our own embryology laboratory and state-of-the-art equipment.
- The medical team holds ESHRE certification.
- We offer a personalised approach for each couple.
- We provide comprehensive support after the procedure.
Talk to an expert about
In Vitro Fertilization

Similar Articles

How Long IVF Treatment Takes: Stages, Timeline and When Results Appear

Belly Injections for IVF: Their Role and How to Administer Them Correctly
