In modern infertility evaluation, transvaginal ultrasound is one of the basic investigations because it quickly provides information about the uterus, endometrium, ovaries and possible causes that may influence the chances of achieving pregnancy. Before initiating an In Vitro Fertilization (IVF) protocol, this examination has a practical role: it helps clarify the medical context and identify situations where additional steps are needed (for example, complementary investigations or treatments before IVF).
This article explains what transvaginal ultrasound can show, how results are interpreted in the context of infertility and the most common aspects assessed before IVF.
What Transvaginal Ultrasound Is and Why It Is Used in Infertility
Transvaginal ultrasound is an ultrasound imaging investigation performed with a special probe inserted intravaginally, allowing detailed visualization of pelvic organs. Compared to abdominal ultrasound, it provides better resolution for the uterus, endometrium and ovaries because the probe is closer to the examined structures.
In infertility evaluation, transvaginal ultrasound is useful both for an “overall picture” at the beginning of investigations and for monitoring at certain moments of the menstrual cycle. In addition, in the context of preparation for IVF, it can highlight situations that influence medical strategy (for example, the presence of an ovarian cyst, suspicion of an endometrial polyp or signs compatible with endometriosis).
When Transvaginal Ultrasound Is Recommended in Infertility Evaluation
In clinical practice, transvaginal ultrasound is frequently recommended in the following situations:
- at the first gynecological evaluation for infertility, as part of a complete gynecological consultation;
- to assess the ovaries and follicles, including ovulation monitoring (depending on the physician’s recommendation);
- before initiating an IVF protocol, to establish a clear imaging baseline;
- when there are symptoms such as pelvic pain, abnormal uterine bleeding or a history suggestive of conditions such as endometriosis or uterine fibroids;
- to follow up on previous findings (for example, an ovarian cyst observed at a prior examination).
Ideally, the indication and timing of the examination are established by the physician according to context (age, medical history, duration of infertility, cycle regularity, associated symptoms and the results of other investigations).
What Information Transvaginal Ultrasound Provides Before IVFansvaginală înainte de FIV
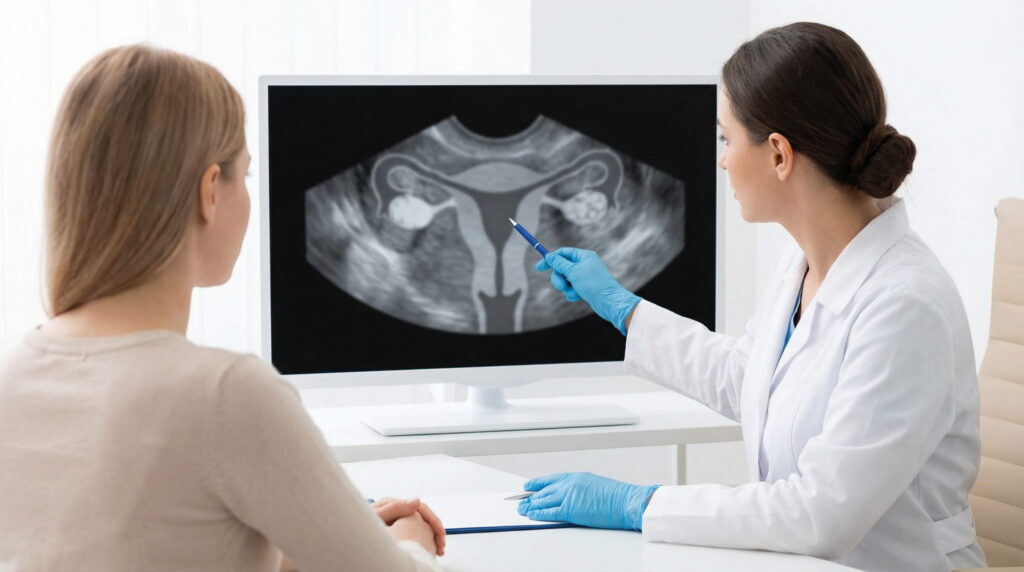
Before IVF, transvaginal ultrasound has a simple objective: to clarify whether there are elements that may influence ovarian stimulation, endometrial quality, embryo implantation or protocol safety. Therefore, interpretation is not done “in isolation”, but correlated with medical history and the rest of the recommended investigations.
The Ovaries: Follicles, Cysts and Signs Suggestive of Endometriosis
The ovaries are evaluated carefully because the IVF plan depends, in part, on anticipated ovarian response. Through transvaginal ultrasound, the following are usually assessed:
- antral follicle count (AFC), a useful imaging indicator in estimating response potential to stimulation (in correlation with hormonal analyses);
- ovarian appearance and possible particularities that may suggest a specific pathology;
- the presence of cystic formations and their characteristics.
An ovarian cyst may have different causes. Some cysts are functional (related to the menstrual cycle) and may disappear spontaneously, while others require follow-up or additional evaluation. In certain situations, the physician may recommend a specific approach before IVF, especially if the formation influences access to follicles, increases discomfort or raises suspicion regarding its nature.
If endometriosis is suspected (for example, an ovarian endometrioma or indirect signs), ultrasound interpretation becomes even more important for planning next steps. In such situations, management may include targeted treatment, depending on severity and objectives, and useful information may be complemented within the endometriosis treatment page.
If a formation requiring treatment is confirmed, options are determined individually. For ovarian cysts with a surgical indication, information about ovarian cyst removal may be relevant, depending on the medical team’s recommendation and the reproductive plan.
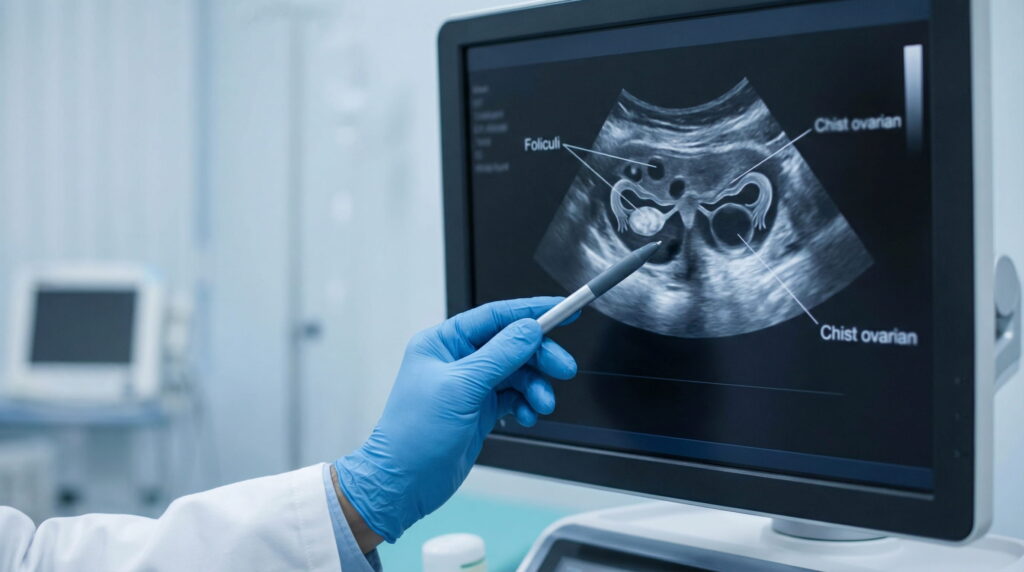
The Uterus: Fibroids, Anatomy and Elements That May Influence Implantation
Uterine evaluation includes shape, dimensions and the presence of lesions that may impact the uterine cavity. A central point is identifying uterine fibroids (myomas) and estimating their relevance in relation to the endometrial cavity.
Not all fibroids influence fertility in the same way. In general, location is essential: a submucosal fibroid or one that distorts the cavity may have a greater impact on implantation than a small subserosal fibroid. In situations where treatment is needed before IVF, the physician may discuss options, and for additional context there is information about uterine fibroid removal.
Transvaginal ultrasound may also raise suspicion regarding certain anatomical particularities (for example, uterine malformations). When more precise clarification is needed, complementary investigations may be recommended (such as sonohysterography, hysteroscopy or MRI), depending on the situation.
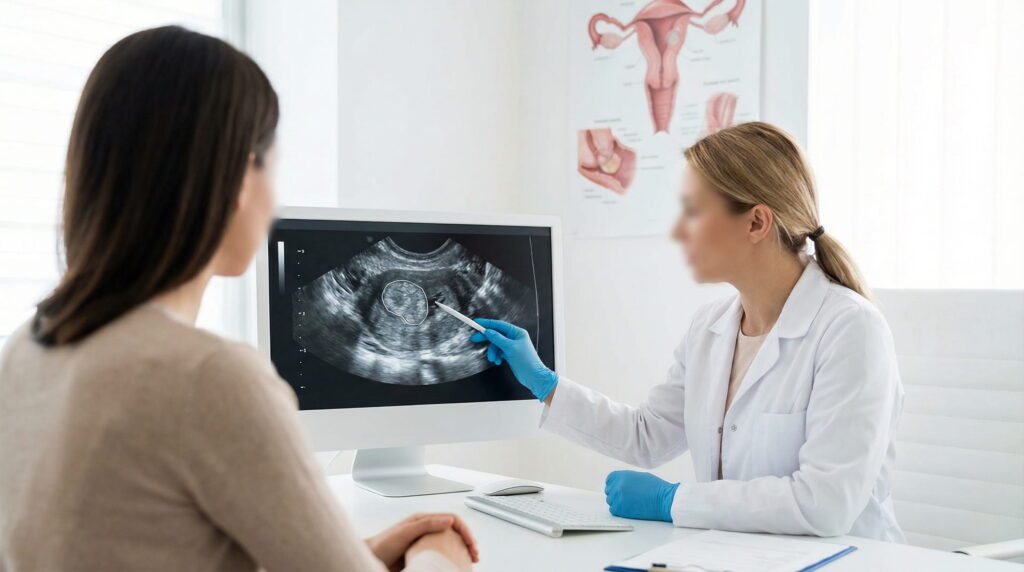
The Endometrium: Thickness, Appearance and Suspected Intracavitary Lesions
Before IVF, the endometrium is evaluated to understand whether there are elements that could influence endometrial receptivity. Transvaginal ultrasound provides information about:
- endometrial thickness (interpreted according to cycle day and context);
- endometrial appearance (pattern), which may guide clinical discussion;
- suspicion of endometrial polyps or other intracavitary lesions.
It is important for these findings to be correlated with examination timing. A thin endometrium on certain cycle days may be physiological, and conclusions relevant for IVF are formulated when the examination is performed at the appropriate time or when repeated monitoring exists.
The Fallopian Tubes and Pelvis: When Ultrasound Suggests Problems That Matter Before IVF
The tubes are not always easy to evaluate directly by ultrasound, but transvaginal ultrasound may suggest certain important situations. One example is suspicion of hydrosalpinx (tubal dilation with fluid), which may negatively influence IVF outcomes in certain contexts and may require management before initiating the protocol.
Also, the presence of fluid in the pouch of Douglas or certain particularities may raise suspicion regarding inflammation, adhesions or endometriosis, aspects that are always interpreted in relation to symptoms and medical history.
When the Ultrasound Result Changes the Plan Before IVF
There are situations where seemingly “small” findings may modify the recommended steps before IVF. Typically, attention is directed toward:
- suspected intracavitary lesions (for example, endometrial polyps);
- fibroids that affect the cavity;
- hydrosalpinx;
- persistent ovarian cysts with characteristics that require evaluation;
- suspicions of clinically relevant endometriosis.
In these cases, management is individualized: sometimes additional investigations are recommended for confirmation, other times treatment before IVF and in certain situations monitoring.
“You deserve to be heard, seen, treated with respect and supported throughout your life.”

Andreas Vythoulkas
Specialist in Obstetrics and Gynecology


On Which Day of the Cycle Transvaginal Ultrasound Is Performed and Why It Matters
Ultrasound timing can significantly influence interpretation. In infertility evaluation, the most frequent recommendations include:
- Days 2–5 of the cycle: useful for “baseline” evaluation, including assessment of antral follicles and identification of persistent cysts.
- The periovulatory period: sometimes used for ovulation monitoring (depending on protocol and objective).
- The second part of the cycle: may be recommended in specific contexts, when certain findings are followed or symptoms are correlated.
In IVF protocols, transvaginal ultrasound may be repeated according to the stages of the medical plan, to guide stimulation decisions and timing.
How You Can Prepare for Transvaginal Ultrasound
As a rule, transvaginal ultrasound does not require complex preparation. In many situations, it is useful for the bladder to be empty and the physician may provide specific instructions depending on context.
For clarity, on the day of examination the following reference points are useful (the list is indicative and adapted to medical recommendations):
- results of previous investigations (ultrasounds, tests, interventions);
- information about the menstrual cycle (date of last menstruation, regularity);
- current medication, if applicable;
- relevant symptoms (pain, bleeding, discomfort).
For information about the service and availability, specific details are centralized on the transvaginal ultrasound page.
How a Transvaginal Ultrasound Is Performed and How Long It Takes
Transvaginal ultrasound is a short investigation. The examination involves using a thin probe covered with a protective sheath, and the physician examines the uterus, endometrium and ovaries in real time on the ultrasound screen.
Usually, discomfort is minimal. However, there may be situations where the examination is more sensitive (for example, in the presence of inflammation, certain cysts, endometriosis or increased sensitivity). In such cases, examination pace and positioning are adapted to maintain comfort.
Limitations of Transvaginal Ultrasound and When Additional Investigations Are Needed
Although transvaginal ultrasound is very valuable, it does not answer all questions by itself. Some situations require completion with additional investigations, chosen according to clinical suspicion.
For example, for a more precise evaluation of the uterine cavity, sonohysterography or hysteroscopy may be recommended, and for clarifying certain suspicions (such as adenomyosis or deep endometriosis) MRI may be useful. For assessing tubal patency, there may be specific indications such as HSG or HyCoSy, depending on the medical plan and objectives.
In the IVF context, these recommendations aim to reduce uncertainties and optimize steps before initiating the protocol. For a broad picture of stages and decisions, the complete IVF guide may also be useful, detailing context and typical process steps.
How the Ultrasound Result Becomes a Plan Before IVF
Interpretation of a transvaginal ultrasound before IVF is not limited to “what is seen”, but to “what it means in context”. The same ultrasound aspect may have different relevance depending on age, symptomatology, history, hormonal analyses and reproductive history.
In short, transvaginal ultrasound may contribute to:
- establishing a correct imaging baseline before stimulation;
- identifying situations that require treatment or additional investigations before IVF;
- adjusting clinical strategy (protocol, timing, monitoring).
In the area of expertise dedicated to IVF, approaches may differ depending on particularities and team preference. In this sense, for the physician’s perspective and for experience-oriented content and explanations, the pages In Vitro Fertilization (IVF) and IVF – patient experience can also be consulted.
Frequently Asked Questions
What does the doctor see on a transvaginal ultrasound?
A transvaginal ultrasound allows evaluation of the uterus, endometrium and ovaries. Depending on cycle timing, ovarian follicles, cysts, fibroids, suspicion of endometrial polyps and other fertility-relevant particularities may be observed.
Can a transvaginal ultrasound show whether ovulation occurs?
It can provide indications through monitoring follicles and ovarian changes over the cycle. Usually, ovulation is correctly assessed through repeated examinations at times established by the physician, sometimes correlated with hormonal tests.
Can ovarian reserve be estimated on ultrasound?
Transvaginal ultrasound can assess antral follicle count (AFC), a useful imaging indicator in estimating ovarian response potential. Interpretation is made together with tests such as AMH and clinical evaluation.
On which day of the cycle is transvaginal ultrasound recommended for infertility?
Frequently, the initial evaluation is done on days 2–5 of the cycle for a “baseline” picture. However, the exact timing depends on the objective: ovulation monitoring, endometrium follow-up or evaluation of previous findings.
Is transvaginal ultrasound painful?
Usually, the examination is well tolerated and short. Discomfort may exist in certain situations (inflammation, endometriosis, painful cysts), in which case the examination is adapted to maintain comfort.
Can the fallopian tubes be seen on transvaginal ultrasound?
The tubes are not always clearly visible, but certain issues may be suggested, such as hydrosalpinx. To evaluate tubal patency, the physician may recommend specific investigations when indicated.
What does it mean if an ovarian cyst is found before IVF?
An ovarian cyst may be functional or may require follow-up and additional evaluation, depending on appearance and persistence. Management before IVF is individualized and may include monitoring, treatment or, in some cases, intervention.
If a fibroid or polyp is discovered, can IVF still be done?
In many situations, yes, but it depends on location and impact on the uterine cavity. Sometimes treatment of the lesion is recommended before IVF to optimize endometrial conditions and implantation chances.

Why Choose Genesis Athens for Transvaginal Ultrasound
In infertility evaluation, examination quality and contextual interpretation make the difference. At Genesis Athens, transvaginal ultrasound is integrated into a clinical approach focused on diagnostic clarity and concrete steps before IVF, when this is the indication established by the medical team.
The examination is performed in a setting where imaging investigations are correlated with medical history, gynecological evaluation and reproductive objectives, so that results are useful for subsequent decisions. For information about the service, evaluation and scheduling, the transvaginal ultrasound page is available, which complements the clinical perspective and how this investigation is integrated into the fertility pathway.
Talk to a specialist about
Transvaginal Ultrasound

Sources:
Similar Articles

When the Pregnancy Test Turns Positive After Implantation Bleeding

IVF Pregnancy by Week: Progress, Symptoms, and Monitoring
